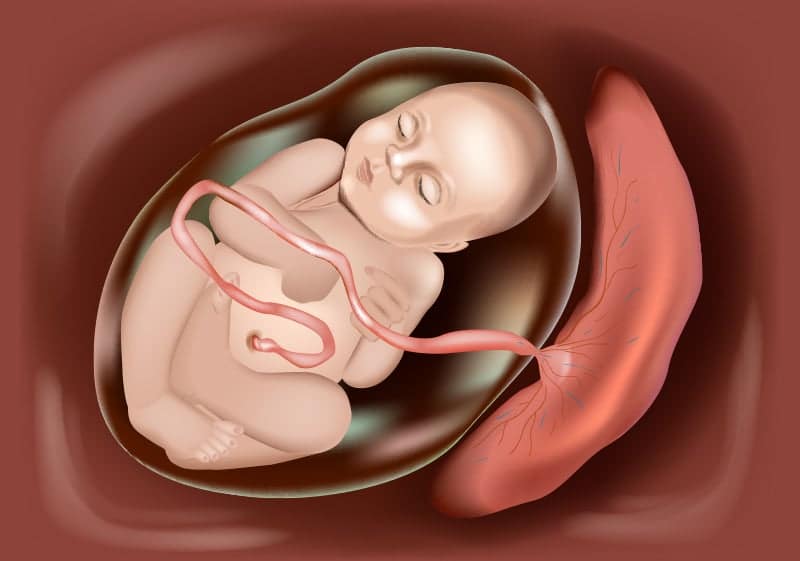
Umbilical Cord:
The umbilical cord, which connects the fetus to the placenta is a biological discard and can be collected at the time of birth without any controversy. The cord tissue/Wharton’s jelly provides a continuous depot of stem cells which can be used for treatment. Wharton’s jelly (WJ) is the connective tissue between the umbilical cord vessels and Umbilical Cord Derived MSCs (UC-MSC), display multipotent characteristics, possess embryonic cell like properties [82] and share more features with fetal MSCs.
“The umbilical cord vessels and surrounding mesenchyme (including the connective tissue matrix that becomes Wharton’s jelly) are derived from extra-embryonic mesoderm and/or embryonic mesoderm. The yolk sac component is the embryologic source of both primordial germ cells and the first hematopoietic stem cells. It is possible that some of these stem cell populations remain behind and co-exist with the mesenchymal stromal cells of Wharton’s jelly. It is also possible that, during development, cells in the Wharton’s jelly migrate into the fetus along with the primordial germ cells and hematopoietic cells to the AGM region.
UCMSCs express MHC Class I but do not express MHC Class II on their surface. They are highly proliferative, possess higher self-renewal capacity compared to adult stem cells (Can and Karahuseyinoglu, 2007), have longer telomers as compared to adult MSCs, can therefore stay stable for longer time periods in culture with minimum risk of genetic alterations. Due to the relative young age and high proliferative capacity, large numbers can be obtained, which could be employed for cell based therapies.
UCMSCs can be induced to form adipose tissue, bone, cartilage, skeletal muscle cells, cardiomyocyte-like cells and neural cells and are usable to tissue engineering applications. Due to their primitive and naive state, these cells do not elicit immune response, hence can be administered allogeneically and are perfect candidates for regenerative cellular treatment compared to Bone Marrow Derived MSCs. Risks of forming
tumors is at a minimum as there is enough evidence in the past findings to support the safety of these cells. UCMCs are immunosuppressive and are known to modulate the dendritic cells and T cells in vivo.
UCMSCs can be isolated from umbilical vein subendothelium and the Wharton’s jelly. There are three regions in the cord tissue where MSCs have been isolated viz. the perivascular zone, the intervascular zone and the subamnion. Wharton’s jelly is the connective tissue surrounding these three regions in the cord tissue. Early evidence by some groups shows that the UC-MSCs isolated from the cord tissue are a heterogeneous mixture of cells originating from the different zones and represent distinct populations.
Studies till date discuss the Wharton’s jelly derived stem cells but detailed characterization of these cells is not properly documented. The differentiation potential of these cells and the percentage of cells committing to a particular cell type is not clear. We speculate that there are subsets of MSCs (mixed populations) present at various stages of multipotency, ranging from undifferentiated fetal like “stem cells” to a more differentiated phenotype.
UC-MSCs can be isolated from any donor, expanded and cryopreserved in allogeneic banks providing a ready source of safe, well characterized committed progenitors for stem cell treatment. Although UC-MSCs have shown promise, lack of detailed characterization of these cells, makes it difficult to proceed further.
Till date the only feasible methods available for large scale harvest of UC-MSCs is enzymatic degradation. This method causes excessive damage to the cord tissue, thereby creating cell lysis and collateral damage. Moreover, enzymes like collagenase will not pass regulatory restrictions for clinical application. Explant method do not result in large numbers of cells plus the time required for the cells to outgrow the explants is long and the cells may senesce in culture. This could be directly related to its telomere length.
These variables will impinge considerably on the study outcome and introduce variability in the system. Due to its heterogeneous nature, differentiation cues which result in commitment of cells is seldom over 25 to 30 % of the total cell population. By employing limiting dilution, one can expand monoclonal populations based on their telomere length and surface markers.
These cells, under differentiation cues will respond uniformly and result in maximum pool of committed progenitors. Studying their surface protein expression at early onset of commitment will display signature profiles for each lineage. Such an approach will increase its therapeutic value in clinical applications. UC-MSC represent an important stem cell population present in the cord tissue, which display multipotent capabilities and are extremely important in regenerative medicine.
Although previous studies have demonstrated its differentiation capacities and stem cell potential, there are certain discrepancies with regard to its biological properties. These differences can be explained by the existence of distinct subpopulations within the cord tissue-derived primary culture which represent functionally distinct cell population. Isolation techniques of UCMSCs use collagenase or protease to digest the extracellular matrix which may alter the function of UCMSCs. Our process patent which does not include enzymatic digestion will circumvent such procedural problems.
As the cord tissue has at least 2 distinct compartments: Wharton’s jelly and the umbilical vein subendothelium, it represents a mixed population of stem cells with varying capacities. Different isolation procedures have led to different cell types, reflecting the heterogeneity of the cord tissue. For example, prechondrocytes were derived from explant cultures of cord tissue, whereas enzymatic digestion of the cord tissue has led to the identification of neural like cells.
Mesenchymal precursor cells were derived by the enzymatic digestion of the Umbilical Cord vasculature endothelial surface. Myofibroblasts were derived from Umbilical Cord vessels or whole cord tissue by mechanical mincing. Studies confirm the presence of myofibroblasts, residing in the Wharton’s jelly which have tested positive for vimentin, desmin and alpha actin.